Scientists with the Georgia Institute of Technology as of late distributed work in Nature Biomedical Engineering that depicts a few new ways to deal with further developing CAR-T, especially for strong tumors.
Vehicle T treatment, like Gilead Sciences’ Yescarta (axicabtagene ciloleucel) for non-Hodgkin lymphoma, intense lymphoblastic leukemia, mantle cell lymphoma and different signs, and Novartis’ Kymriah (tisagenlecleucel), supported for intense lymphoblastic leukemia, ongoing lymphoid leukemia, diffuse huge B-cell lymphoma, just as others, are exceptionally successful for hematologic malignant growths. Nonetheless, getting CAR-T to work in strong tumors has been a harder nut to open.
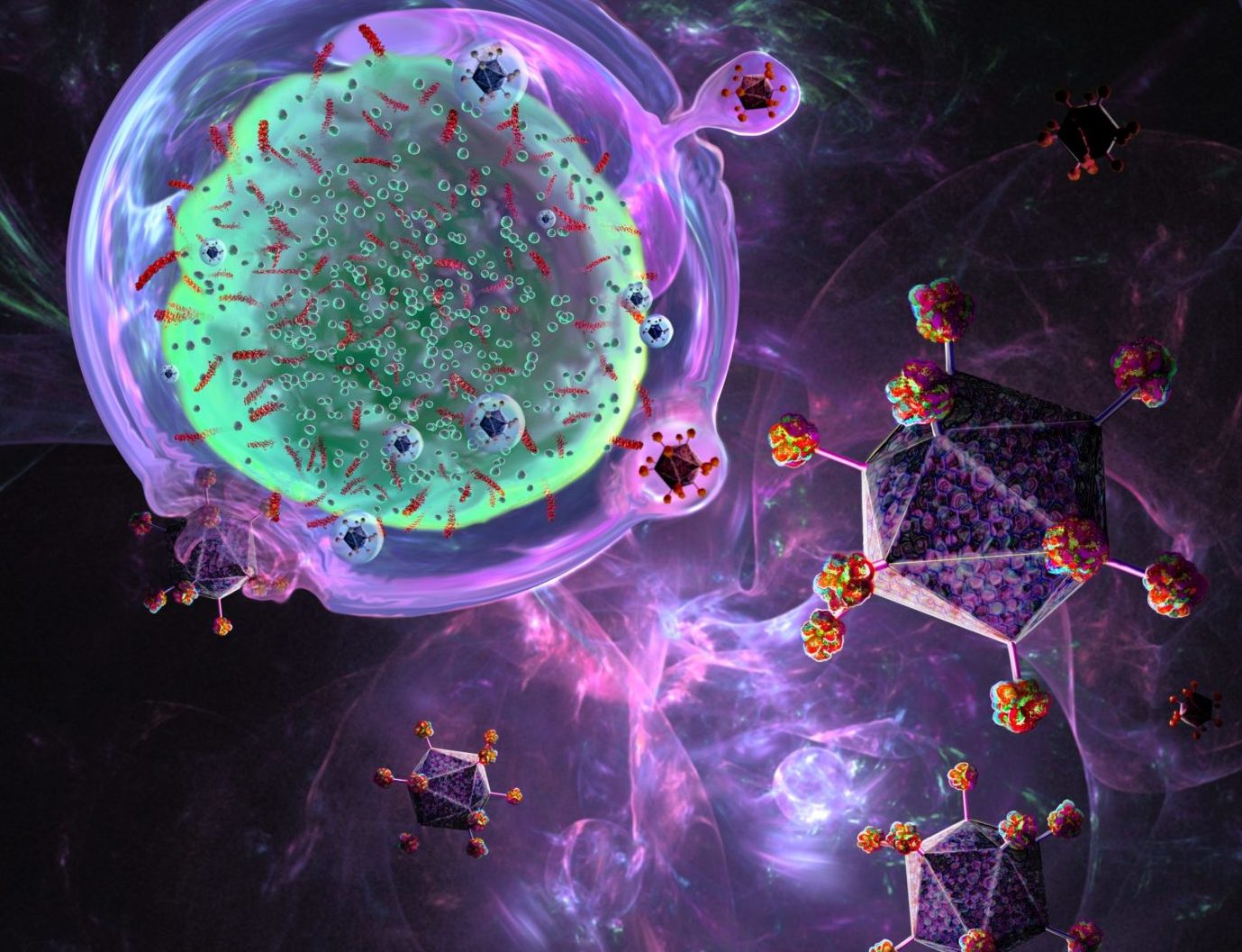
In CAR-T (illusory antigen receptor T-cell) treatment, T-cells are segregated from a malignancy patient, designed in the research facility by adding a quality for a fanciful antigen receptor (CAR), developed, then, at that point implanted once again into the patient. There, they become a kind of living treatment profoundly tuned to assault the patient’s malignancy.
“These treatments have demonstrated to be strikingly viable for patients with fluid tumors — in this way, tumors that are flowing in the blood, like leukemia,” Gave Kwong, partner educator in the Wallace H. Coulter Department of biomedical designing at Georgia Tech and Emory, and senior examination examiner disclosed to Genetic Engineering and Biotechnology News.
“Sadly, for strong tumors — sarcomas, carcinomas — they don’t function admirably. There are various reasons why. One gigantic issue is that the CAR T-cells are immunosuppressed by the tumor microenvironment.” Kwong’s group is attempting to change the microenvironment to further develop CAR-T in these diseases. One methodology is to make an on-off switch that is touchy to warm.
Prior work directed by his exploration bunch absolutely targets tumors with a neighborhood store of warmth, which actuates the CAR-T cells inside the tumor. To make heat, they utilized laser beats from outside the body.
Gold nanorods that are conveyed to the tumor convert the light waves into restricted warmth, expanding the temperature to 40 to 42 degrees C, which actuates the switch however doesn’t hurt sound tissues or the T-cells. As well as hereditarily designing the CAR-T cells to react to that switch, they have additionally overhauled them to produces insusceptible stimulatory particles. These cytokines and bispecific T-cell engagers are controlled cautiously.
Kwong said, “These malignancy battling proteins are great at invigorating CAR T-cells, however they are too harmful to be in any way utilized outside of tumors. They are too poisonous to even think about being conveyed foundationally.

Yet, with our methodology, we can limit these proteins securely. We get every one of the advantages without the downsides.” The investigation was led on mice. The exploration prompted a 60-overlay higher articulation of a columnist transgene without influencing the CAR-T cells’ multiplication, relocation, and cytotoxicity.
The framework restored disease in the mice, contracting tumors and forestalling backslide. The scientists say that when they test it in people, rather than the laser, they will utilize centered ultrasound, which is noninvasive while focusing on any area in the body. Lasers don’t enter far enough into the body to be a reasonable methodology in people.
“So,” Kwong said, “in the event that you have a profound situated harmful tumor, that would be an issue. We need to kill issues.”
___________
Tumor | Don’t forget to follow us on Twitter @njtimesofficial. To get the latest updates