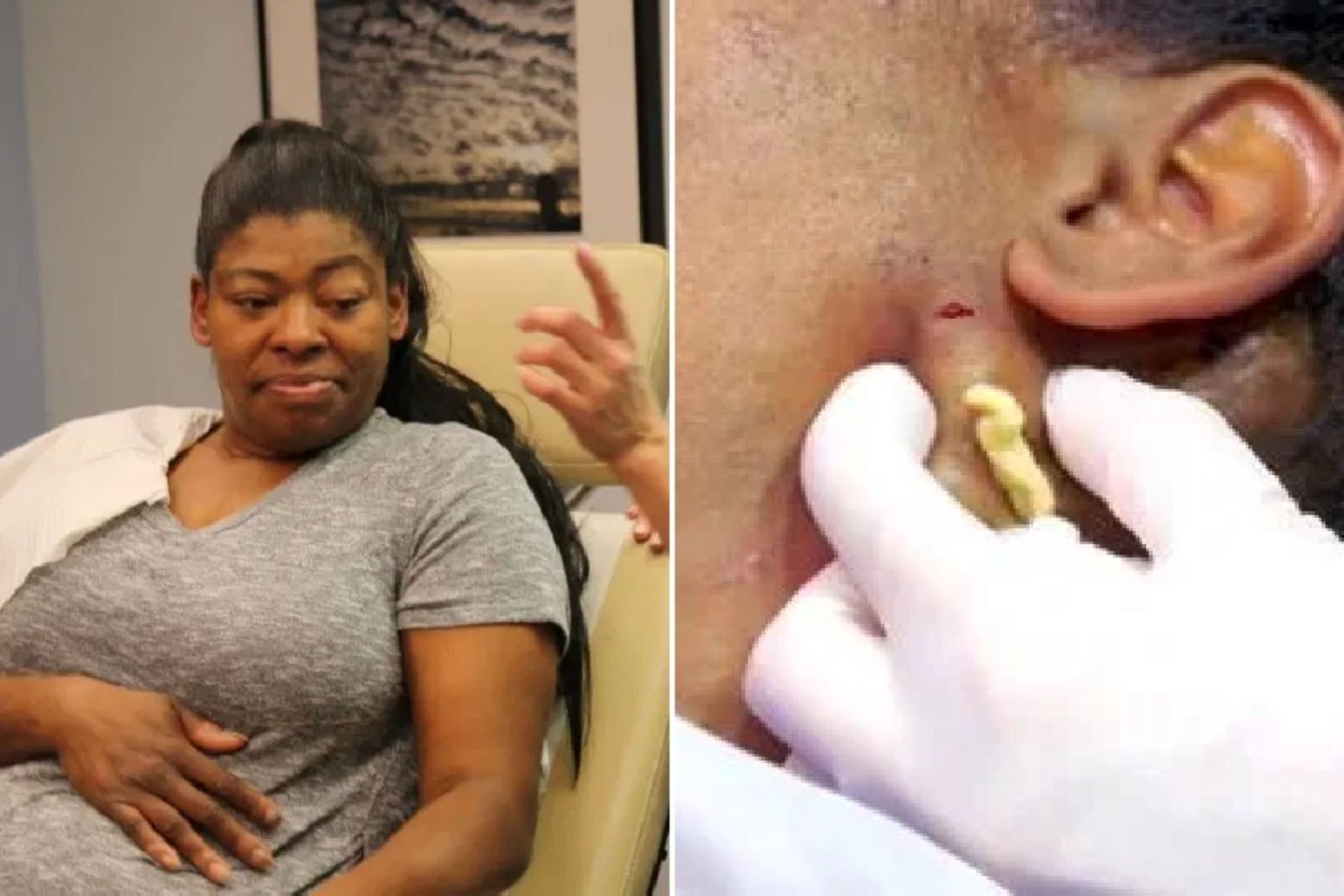
COVID-19 patients, the Indian government advised physicians to look at signs of mucormycosis, also called black fungi, as hospitals report increased cases of rare but potentially fatal infections.
First case of mucromycosis in Madhya Pradesh region of India has been reported as the patient named DR. Pratap Singh Verma shared his experience stating that he had lost his vision and blood clotting has been recently stopped by the doctors after performing the surgery so that the infection might not get into patients brain and thus causing the person to be brain dead but the patient is still not considered out of danger.
According to the state-run Indian Council of Medical Research (ICMR), doctors in COVID-19, diabetics and patients with impaired immune systems should consider early symptoms such as sinus paint or nasal blockage on one side of the face, unilateral headaches, swelling or numbness, toothache or tooth loosening.
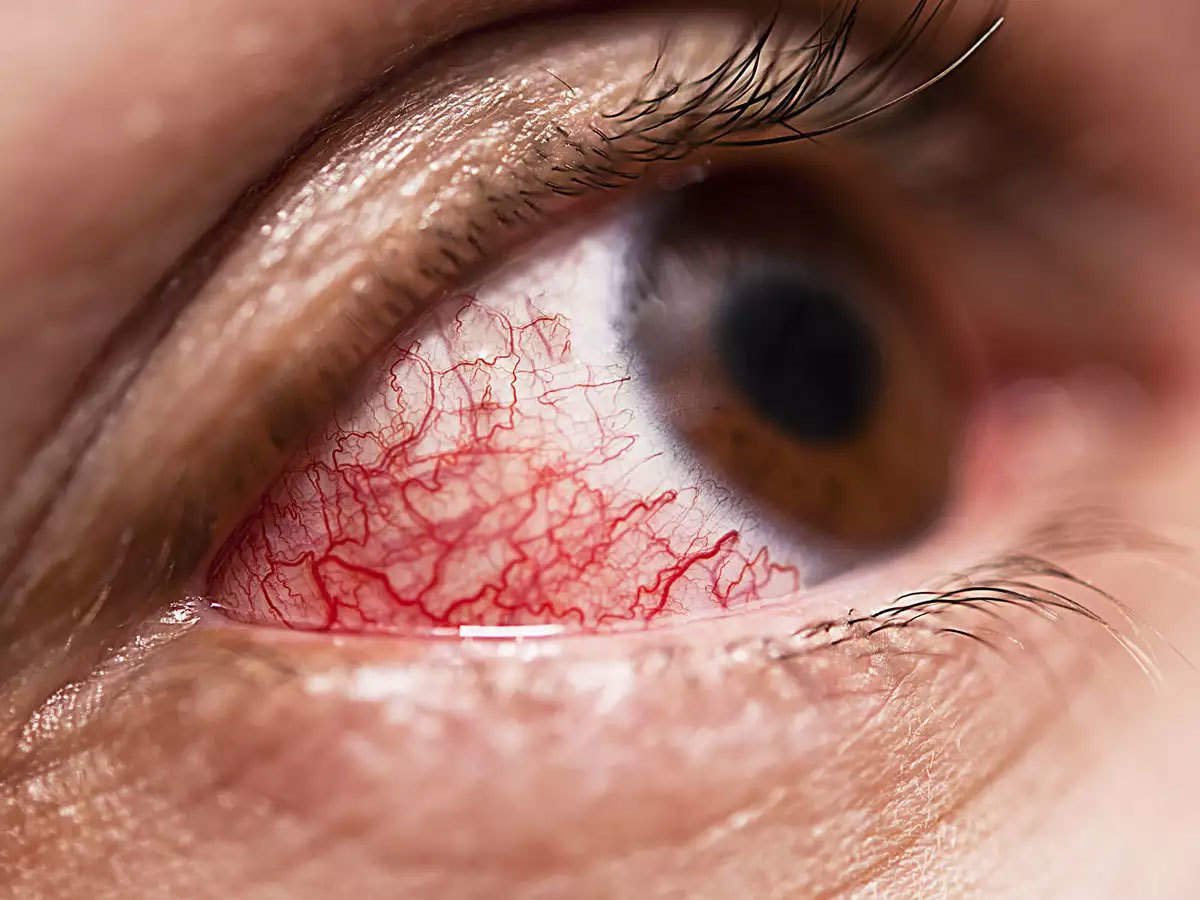
Diabetes is strongly associated with disease that can cause nasal discolouration, blurred and double vision, chest pain, difficulties in breathing, and coughing of the blood. Steroids like dexamethasone that is used to treat severe COVID-19 may exacerbate diabetes.
“There have been cases reported in several other countries, including the United Kingdom, the United States, France, Austria, Brazil, and Mexico, but the volume is much higher in India,” said David Denning, a professor at the United Kingdom’s Manchester University and an expert at the Global Action Fund for Fungal Infections (GAFFI).
“One of the reasons is that there is a lot of diabetes, and a lot of poorly controlled diabetes.”
Although India has not published national data on mucormycosis, the country has stated that there is no major outbreak. According to media reports, there have been cases in Maharashtra and its capital, Mumbai, as well as Gujarat.
“It’s not something to panic about,” said Aparna Mukherjee, an ICMR scientist. “But you have to be aware of when to seek consultation.”
However, it is a complication that India’s overburdened hospitals could do without, as they are desperately short of beds as well as the oxygen required for severely ill COVID-19 patients.
Mucormycosis was more common in India than in most other countries, according to Arunaloke Chakrabarti, director of the Center of Advanced Research in Medical Mycology in the Indian city of Chandigarh and a GAFFI adviser, even before COVID-19, “partly because of the millions who have diabetes.”
According to him, severe cases may necessitate specific antifungal therapy as well as multiple operations.
P Suresh, head of opthalmology at Fortis Hospital in Mulund, Mumbai, said his hospital had treated at least ten such patients in the previous two weeks, roughly twice as many as in the entire year preceding the pandemic.
All had COVID-19 infection, and the majority were diabetic or had received immunosuppressive drugs. Some had died, and others had lost their sight, he explained. Other doctors reported a similar increase in cases.
“Previously, if I saw one patient a year, I now see about one a week,” said Nishant Kumar, a consultant ophthalmologist at Hinduja hospital in Mumbai, referring to the potential for contamination of hospital oxygen pipes and humidifiers.
Denning referred to it as a “triple whammy.” “You have a high rate of mucormycosis, a lot of steroids – perhaps too much – being used, and then you have diabetes that is not well controlled or managed.”
_____________________
Mucormycosis | Don’t forget to follow us on Twitter @njtimesofficial. To get latest updates